
In a small district hospital, a doctor finishes an emergency CT scan at midnight. There is no radiologist on-site. Within minutes, the images travel through a secure network to a radiologist sitting in another city. The report arrives before the patient’s family can even worry. The treatment begins immediately.
This simple story shows what a remote radiology workflow can do. It removes the limits of distance and time. Hospitals in rural or understaffed regions can still deliver expert diagnosis through connected systems like PACS and cloud teleradiology. Today, this approach is not a luxury but a lifeline for modern healthcare. Mediog uses this same workflow to make diagnosis faster, safer, and easier for hospitals everywhere, bridging people, data, and decisions in real time.
How Remote Radiology Workflow Solves Distance in Diagnosis
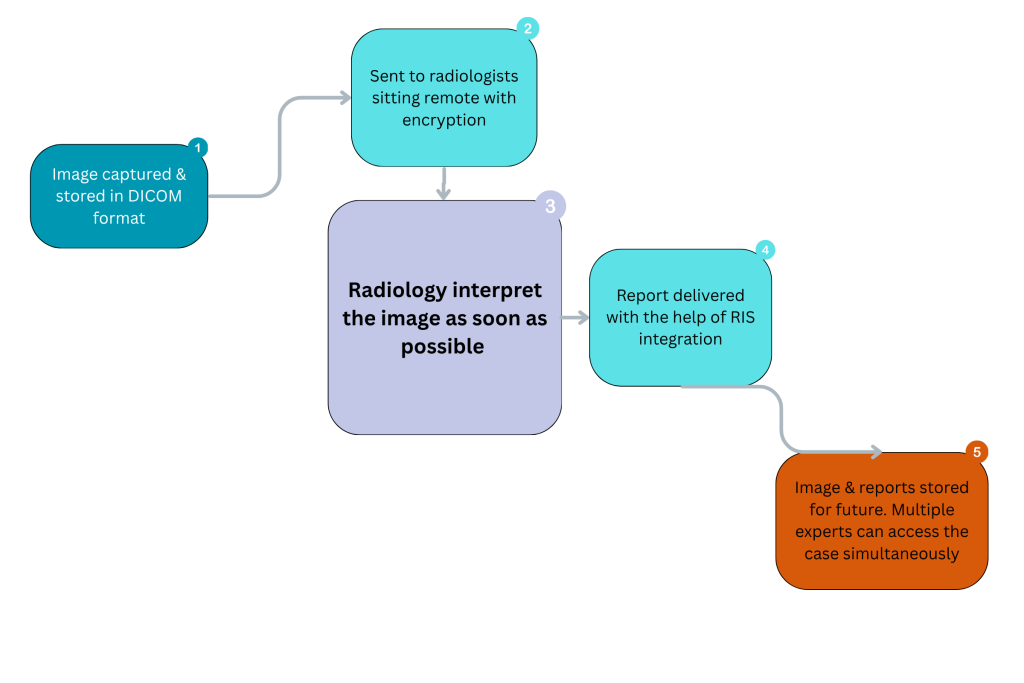
The remote radiology workflow connects imaging sites and radiologists through a secure digital network that eliminates the limits of geography. It replaces manual image transfers with automated cloud-based sharing, ensuring rapid report delivery and expert collaboration. Each stage of this system plays a role in improving diagnosis speed, accuracy, and communication. Mediog follows the same workflow within its teleradiology PACS system, enabling hospitals to receive accurate reports quickly, even in locations with no on-site radiologists.
Step 1: Image Acquisition at the Hospital
Every workflow begins with a patient scan, CT, MRI, or X-ray, captured under diagnostic standards by trained technologists. These are stored in DICOM format, ensuring consistent quality across systems. If the facility only uses film-based machines, the images can be digitized using scanners or cameras, as successfully done in India’s Tripura region, where 26 rural hospitals shared scans remotely with radiologists hundreds of kilometers away (Source: International Journal of Health Technology and Innovation).
In Mediog’s system, these images are uploaded directly to a cloud PACS immediately after acquisition, allowing radiologists to access them securely without physical transfer delays.
Step 2: Secure Image Transmission & Storage
Once the scans are captured, they are transmitted to remote radiologists through encrypted and HIPAA-compliant channels. Modern platforms use cloud-based PACS to ensure lossless data transfer and maintain patient confidentiality. According to the report, using DICOM and encrypted servers prevents unauthorized access and supports interoperability between hospitals and remote specialists (Source: RAD365).
Mediog’s remote radiology reporting services use the same principle; every file remains secure, traceable, and instantly retrievable for future reviews, even in low-bandwidth regions.
Step 3: Remote Interpretation by Radiologists
Radiologists log in to view images using high-resolution diagnostic workstations. They can zoom, measure, and reconstruct images in 3D for precise evaluation. Some advanced systems, including Mediog’s, integrate AI triage tools that flag urgent cases such as brain bleeds or fractures for priority review, ensuring critical reports are issued within minutes.
In practice, teleradiology platforms around the world now achieve turnaround times of 2–3 hours for routine cases and 15–30 minutes for emergencies, according to studies across Africa and the U.S. (Source: PMC PubMed Central).
This combination of technology and expertise lets hospitals receive subspecialty-level reporting without delays, improving care quality even in remote locations.
Step 4: Report Delivery and RIS Integration
After analysis, the radiologist’s report is automatically sent back to the hospital. In Mediog’s PACS and RIS integration, the report appears directly in the patient’s Electronic Health Record (EHR) or hospital dashboard. This instant delivery shortens communication gaps between radiologists and clinicians.
Evidence shows that linking PACS with RIS improves overall report turnaround by up to 90%, as seen in Ethiopian hospitals where teleradiology reduced waiting times from 43.5 hours to 4.6 hours and improved patient satisfaction by 11%. (Source: PMC PubMed Central)
Step 5: Real-Time Collaboration and Interventional Support
Beyond reading images, remote radiology allows live case discussions between radiologists and physicians. Multiple experts can access the same case simultaneously to provide remote interventional radiology support for urgent decisions.
For hospitals that lack subspecialists, this is transformative; a rural clinic can consult a pediatric neuroradiologist or trauma imaging expert instantly through the same network (Source: NHS England). Mediog’s system is built around this connected model, offering hospitals the ability to invite external specialists securely into their ongoing diagnostic process.
Together, these steps form a unified remote radiology workflow that removes physical barriers from diagnosis. It improves reporting efficiency, optimizes radiologist availability, and enhances care quality for patients regardless of where they live.
Conclusion
Radiology is no longer confined by walls or waiting rooms. The shift toward remote radiology workflow has shown that expertise can travel faster than distance itself. What once required physical presence can now be done securely, collaboratively, and in real time.
Hospitals today stand at a turning point; they can either continue operating within the limits of local availability or move toward a connected model that ensures uninterrupted diagnostic service. Mediog offers that bridge. By combining cloud-based PACS, RIS integration, and secure teleradiology reporting, it helps hospitals deliver accurate diagnosis to every patient, regardless of where they are. The path to modern, borderless healthcare is already here, and Mediog makes it practical, efficient, and ready for the next generation of medical care.
###